Ashley Wright, Canowindra Soldiers Memorial Hospital
About
Canowindra Soldiers Memorial Hospital is a 15 bed facility in Western NSW Local Health District, located 60km from Orange NSW, and a hub within the beautiful rural community of Canowindra.
The multidisciplinary team that worked on falls prevention as part of the CEC's Leading Better Value Care Falls in Hospital Collaborative was Ashley Wright, Tara Bushell, Amara Flannery, Raelene Warn, Anumol Philip, Renee Guihot, Dr Padma Madduru, Janice Rumph, Sharon McKay, Shelley Moor, and Jenny Boyton with Ingrid Hutchinson and Evette Buono from the CEC providing coaching and support.
What they achieved
The team's aim in the CEC Falls in Hospital Collaborative was to ensure that 90% of patients aged 70 years and over, admitted to Canowindra Soldiers Memorial Hospital, had a fully completed Falls Risk Assessment and Management Plan (FRAMP) within 24 hours of admission.
The team used a cause and effect diagram to brainstorm the possible causes of delays in completion of falls risk assessments. They designed and undertook a series of Plan Do Study Act (PDSA) cycles to address the possible causes. The PDSAs that were most effective were incorporating discussion about patient falls risk and 'days since last fall' at the daily safety huddles, and adding a prompt to handover sheets (which then became electronic patient journey boards) to highlight falls risk and management plans.
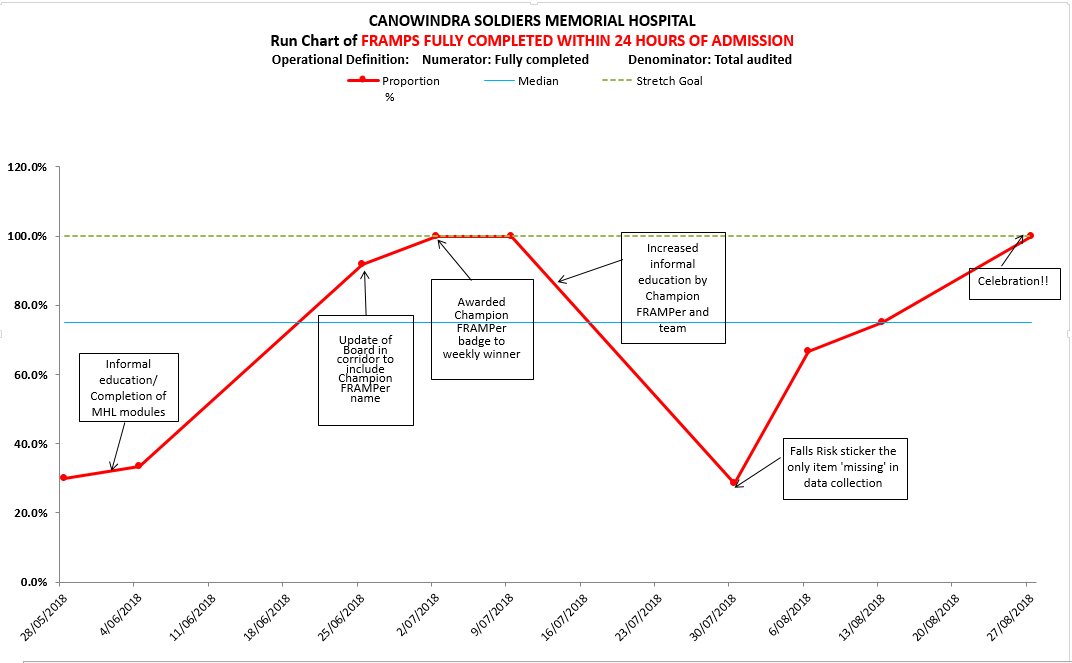
The team kept a close eye on their measurement strategy, displaying their run charts and 'days since last fall' on their 'Staying Safe & On Your Feet' noticeboard. To promote positive change, the team celebrated small wins including reaching their first 50 days since the last fall with a delicious home-baked chocolate cake!
Canowindra Soldiers Memorial Hospital have reached their aim of 90% of FRAMPs being completed within 24 hours on several occasions during the Falls in Hospital Collaborative. They are now working towards achieving 95% reliability.

We spoke to Ashley Wright, Team Leader, at the conclusion of the Falls in Hospital Collaborative about her experience and what she learned.
What are the three things that have had the greatest impact on this quality improvement work?
The three things that have had the greatest impact are the tools that we have learnt about to take back to our teams, the crossover in how the little changes that we've made have affected other things in the hospital and also the team approach - the value of getting the whole team on board to do those things.
What effect has your involvement in this collaborative had on your patients?
The effect our involvement has had on patients has been amazing we think. We need to analyse that more but overall because it has had such a positive effect on staff you can see that coming through in the patients. We have asked some of them and they have been very positive about that new culture and attitude.
If you were to do this collaborative all over again – what would you do differently?
Communicate to the whole team early. We didn't really know what we were doing initially, but once we worked that out, that became much better.
Do you think you can apply the QI methodology that you've learnt to other areas? How so?
Yes, enabling the whole team and all the staff members to be able to use these approaches would be fabulous for patient care. The greatest impact has been the cultural change in our hospital.
More on falls prevention
The Clinical Excellence Commission has been working with eHealth NSW to integrate falls risk assessment and management into a comprehensive care online pathway used when patients are transferred to hospital, providing guidance for more holistic and person-care care.
Strategies and tools for falls risk screening and prevention.

