Edward Davidson, Coledale Hospital
About
Coledale Hospital is a small hospital specialising in rehabilitation and aged care services for the northern Illawarra. It is located at a spectacular beachside location south of Sydney and north of Wollongong.
The team from Coledale Rehabilitation ward that participated in the CEC Leading Better Value Care Falls in Hospital Collaborative included team leader and physiotherapist Edward Davidson, Suzanne Lide, Lisa-Gaye Beauchamp, Kim Harvey, Rochelle Pauw, Tatjana Radmanovic, Melissa Ransley-Hornung, Liam Sharp, and Terena Williams.

What they achieved
The multidisciplinary team's aim was to improve reliable completion of intentional rounding (using the 5Ps model) to reduce the risk of falls at Coledale. A flowchart was used to look at the patient's journey and points of interaction with different staff, identifying areas for improvement.
A series of Plan Do Study Act (PDSA) cycles were used to test changes and assess if they were resulting in improvement. Importantly, patients were involved and were asked about the current 5P process (asking about pain, position, personal care, personal environment, and performing a scheduled task) and indicated they did not like being asked about personal things using a routine script. Instead, patients preferred being offered general help with each encounter with staff. This led to a change whereby everyone in the team (clinical and non clinical staff) was empowered and encouraged to answer the patient's call and ask them "Are you okay?", or asking "Is there anything else I can get you before I go".
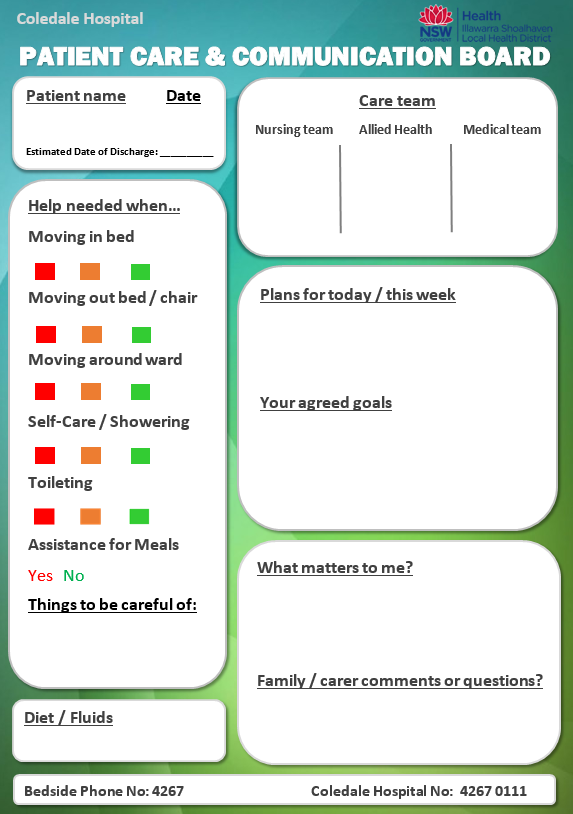
Patient Care and Communication Boards were also redesigned, made larger, used more patient focused language, included goal setting and both patients and their families were encouraged to contribute to the board.
Other changes including making improvements to night lighting, as well as providing updates and feedback on PDSAs during each shift's Safety Huddle. The team also tested mobile work stations (PODs) positioned throughout each ward. Utilising existing Workstations on Wheels (WOWs), they placed a two-way-radio on each WOW for direct and immediate communication between staff and teams for assistance. This resulted in nursing staff have moved away from the nurses station to patient care areas.

Between July 2017 to July 2018, these changes contributed to a 30% reduction in the falls rate (from 6.1 to 4.3 falls per 1000 bed days) in the Rehabilitation ward at Coledale Hospital.

We spoke to Edward Davidson, Team Leader, at the conclusion of the Falls in Hospital Collaborative about his experience and what he learned.
What are the three things that have had the greatest impact on this quality improvement work?
We brought a multidisciplinary team together to enact changes on the ward at Coledale Hospital, bringing the team together to share the problem. Three things that made the most difference have been our ways of working with:
- introduction of pod stations (moving nurses closer to the patient)
- revised patient care and communication boards
- streamlining processes to [support] intentional rounding, across all non-clinical and clinical teams on site.
What do you think were your greatest barriers for this quality improvement work?
The greatest barriers to begin the quality improvement work has been the time needed to respect the methodology, so we're doing the right thing to make a difference to process rather than jumping straight into action. We needed to bring everybody together and we held staff open forums to bring in all the staff on rotation on different shifts. This was important to ensure we're on the same page and we're sharing the problem.
What effect has your involvement in this collaborative had on your patients?
We found our patients felt more supported and were more engaged in their care. They're willing to speak up and use the call bell. When traditionally, they have been less willing to bother staff, but knowing that staff are always there to answer their call has made a great difference to our ability to deliver care and meet their needs. One patient commented, "It's nice to know that someone is close by if you need anything or you're in crisis".
If you want to do this collaborative all over again, what would you do differently?
I would bring a friend. I also would spend some more time defining our process, outcome and balancing measures, ensuring that processes are measured reliably. I think defining process measures was quite a difficult step to take for myself.
Have you had good engagement with other team members from a multidisciplinary perspective?
We've had great engagement from the multidisciplinary team, and have further strengthened the teamwork and collaboration across Coledale hospital. It's important to recognise the active support from our executive - our DON – which has been fantastic across our non-clinical and clinical teams. At each shift's safety huddle we bring in all multidisciplinary team members to communicate and share our problems and successes, alongside the daily staff and patient safety plans and events for the day.
Do you think you can apply the QI methodology that you've learnt to other areas? How so?
Absolutely, we can apply this QI methodology ongoing with the work needed here and, scale the use of the QI tools learned into all levels of quality improvement work in the future. We've got two wards with different needs and workflows at Coledale hospital and, there's still a lot more to do here in achieving good outcomes. We have to ensure reliability of our processes are sustained before we move on and adjust processes to implement and measure on the next ward.
More on falls prevention
The Clinical Excellence Commission has an extensive collection of resources on falls prevention.
More on safety fundamentals for teams
Safety Fundamentals are activities that focus on strengthening behaviours that impact safe and quality care, and are associated with a positive impact in staff and patient experience. Safety Huddles, Leadership WalkArounds, intentional rounding and multidisciplinary team rounds are all safety fundamentals.
