End of Life
Each year nearly 50% of people who die in NSW die in NSW acute care facilities. A common concern highlighted in many incident reports is the failure of treating teams to identify patients at risk of dying, and then develop and document appropriate treatment plans and communicate appropriately with patients and carers.
Overview
The CEC End of Life program has an important role in the state-wide approach to EOL care and supports the delivery of the five priority areas outlined in the NSW Ministry of Health document - End of Life and Palliative Care Framework 2019-2024 and other EOL and palliative care programs in NSW.
The CEC programs include the AMBER care bundle, the Last Days of Life toolkit and a statewide mortality review process.
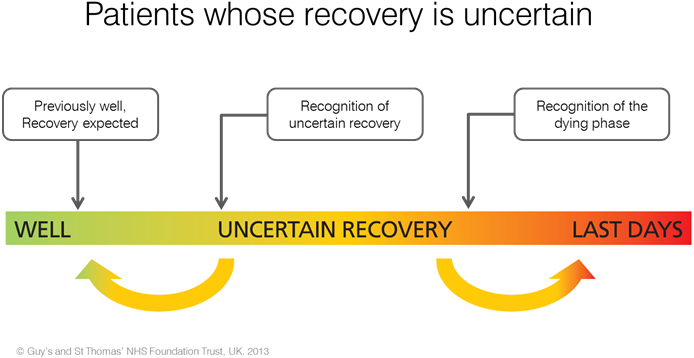
The AMBER care bundle is a systematic approach for the multidisciplinary team to follow when clinicians are uncertain whether a patient may recover. It encourages clinicians, patients and families to continue with treatment, in the hope of a recovery, whilst talking openly about preferences and wishes, and putting plans in place in preparing for end of life.
The AMBER care bundle toolkit is made up of resources and tools to guide local health districts (LHDs) and healthcare facility staff in the preparation and implementation of the AMBER care bundle.
To improve and support the care of the dying patient, the CEC, in collaboration with clinicians and consumer advisors, developed the Last Days of Life toolkit.
The toolkit provides tools and resources to ensure all dying patients are recognised early receive optimal symptom control, have social, spiritual and cultural needs addressed, both patient and families/carers are involved in decision-making, and bereavement support occurs.
The tools have been specifically developed for use by generalist clinicians and are not intended to replace either local Specialist Palliative Care guidelines or advice given by Specialist Palliative Care clinicians.
The various tools developed relate to:
- Recognition of the dying patient, management planning and care after death;
- Medication prescribing for symptom management;
- Accelerated transfer to die at home;
- Communication.
Mortality review is a process in which the circumstances surrounding the care of a patient who died during hospitalisation are systematically examined. The CEC, in consultation with clinicians, has developed a death screening tool and database. This provides NSW local health districts and speciality networks with a standardised, best-practice method of screening and reporting on all in-hospital patient deaths.

