Health literacy
In Australia, 60% of people have low health literacy [1]. Health literacy describes how people access, understand, appraise and apply health information in order to make decisions about their health [2]. Partnering with patients, families and carers to ensure understanding of their health can reduce personal, community and economic costs of care.
It is important to address health literacy across the whole health system in order to deliver care which is safe, high quality and person centered. Change at both individual and organisational levels is needed.
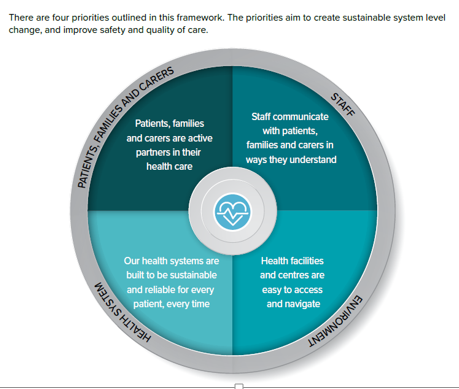
The CEC has developed a Health Literacy Framework as a guide to action. There are four priorities outlined in the framework. The priorities aim to create sustainable system level change, and improve safety and quality of care.
Enabling patients, families and carers to understand and manage their health is a key way to improve their quality of life and reduce the impact of disease. Identifying and removing barriers for them to become active partners in their health care is vital.
- NSW Health Literacy Framework - A guide to action
NSW Health Literacy Priorities
It can be difficult to know where to start your health literacy journey. The following tools may help:
- Do a gap analysis of the Ten Attributes of Health Literate Health Care Organisations using the tool developed by NNSW LHD and now available on QARS (Quality Audit Reporting System).
- Refer to the Matrix to view links between Ten Attributes, framework priorities and national standards.
- Define your goals – ensure they are SMART (specific, measurable, achievable, results, time bound) – see Quality Improvement Academy for improvement tools.
- Take a system's approach to producing consumer resources. Follow the process outlined by ISLHD, and available on the WSLHD health literacy site. See also CEC plain English writing tips reference.
- Ensure your health centres and facilities are easy to access and navigate by doing regular audits using the QARS tool.
- Translating resource material – ensure your English copy is written in plain English prior to seeking translation.
The NSW Health Literacy framework recommends the use of universal precautions for health literacy. This means providing easy to read information for all, regardless of their health literacy level, and ensuring understanding by using Teach Back.
Should you wish to measure individual or community health literacy, there are a range of tools that exist. Measuring your organisation’s responsiveness to health literacy needs is recommended.
The Health Literacy Tool Shed is an online database of tools that measure individual health literacy. It contains information based on peer reviewed literature - There are more than 100 measures on the site, including:
- Rapid Estimate of Adult Literacy in Medicine (REALM),
- Test of Functional Health Literacy in Adults (TOFHLA)
- Newest Vital Sign (NVS).
Note that many measures are not freely available, but need to be requested from authors.
The Ophelia approach to optimising health literacy, from Deakin University, is a system that supports the identification of community health literacy needs, and the development and testing of potential solutions. It allows easy application of evidence-based health promotion approaches to the field of health literacy. Measurement tools include:
- The Health Literacy Questionnaire (HLQ) identifies the specific health literacy strengths and limitations of people and communities. It examines nine areas of health literacy.
- The Conversational Health Literacy Tool (CHAT) tool was co-developed by Deakin University and healthcare providers to assist in the assessment of their client’s health literacy strengths and needs.
- The Information and Support for Health Actions Questionnaire (Isha-Q ) has been designed for cultures in which decision making about health is often a communal activity.
- The organisational responsiveness (Org-HLR) framework to describe the characteristics of health literacy responsive organisations.
The Patient Education Materials Assessment Tool (PEMAT) can be used to assess the understandability and actionability of print and audiovisual patient education materials. See the tool and user guide on Agency for Healthcare Research and Quality
The Suitability of Materials (SAM) tool scores materials in six categories: content, literacy demand, graphics, layout and typography, learning stimulation and cultural appropriateness. Even materials written on a low grade level may be difficult to comprehend if proper attention is not also paid to organization, layout, and design. The SAM yields final percentage score. This score falls into one of three categories: superior, adequate or not suitable.
The SAM can be used to identify specific shortcomings that reduce the suitability of materials- either in the development stages or with existing materials. Although the SAM was developed for use with print materials, it has also been used to assess video- and audio-taped instructions to patients.
The following tools can help patients, families and carers to communicate with their doctor, nurse or other health professional.
- Ask flyer
- Ask question card
- Ask Consultation summary
- Choosing Wisely Australia
- Five questions to ask your doctor before a test, treatment or procedure
- Healthdirect Question builder.
The question builder helps you prepare for your medical appointment by creating a list of questions to ask. There are other useful resources on the site, including a symptom checker and health information.
The links below profile the experiences, tools and resources of various Local Health Districts (LHDs) in improving health literacy. They are available as reference materials for NSW Health facilities. All intellectual property remains that of the LHD or facility. If you would like to use, adapt or modify them, please contact the LHD or facility.
[1] Australian Bureau of Statistics, 2009.
[2] Kickbusch, I, et al. (eds). The Solid Facts. World Health Organization: 2013.
